On January 6th, the Centers for Medicare and Medicaid Services (CMS) released Part I, CMS-HCC Risk Adjustment Model of the Advanced Notice of Methodological Changes for Calendar Year 2021 (Notice). Part II will be published by early next month with both parts finalized by April 6th. This Notice continues the changes in risk adjustment introduced as part of the 21st Century Cures Act (Act).
Background and Changes
As background, CMS utilizes risk adjustment to account for the variations in conditions that exist across a plan’s population. Knowing that plans will experience this variation, and the bid may not fully cover the cost of treating certain populations, CMS utilizes risk adjustment to prospectively pay plans for enrollees that cost more. There has been criticism, culminating with the changes in the 21st Century Cures Act, that risk adjustment allows plans to overinflate an enrollee’s conditions increasing the payment to the plan. The changes in the Act phase in a new model through which risk adjustment is calculated.
Historically, the CMS-HCC Model utilized diagnosis codes to assign conditions into certain categories and predict the cost of care. It also pulled in enrollee demographics since that may create variability in the cost of care. These demographics and conditions ultimately create a multiplier (coefficient) for the base capitated rate with payment being adjusted based on these coefficients. The coefficients are additive in that the more conditions (and sub-conditions) that an enrollee has as part of a diagnosis, the greater the payment adjustment.
The Act requires phased-in risk adjustment changes utilizing the Alternative Payment Condition Count (APCC) model, which was designed to create a more precise and less prone to overpayment approach. It moves the calculation from one where CMS utilized diagnosis information submitted by plans, as described above (2019 Model), to also including encounter data captured as part of a patient visit (2020 Model). These changes are phased in over a 3-year period, which began in 2019 with full implementation by 2022.
When rolled out, the risk adjustment model was a blend of the new and old methodology. In the first year, 75% of the risk score was calculated utilizing the 2019 model and 25% the 2020 model. CY20 blended the risk score with 50% from the 2019 model and 50% from the 2020 model.
The changes announced on January 6th move the blend for CY21 with 25% of the risk score using the 2019 model and 75% of the risk score from the 2020 model. This has implications for plan payments because in many cases it causes a downward adjustment in the risk score and corresponding plan payment.
The following is an example that demonstrates the impact of this change:
Medicare payments capitated rate = base $ amount x beneficiary-specific risk score (RAF)
Example:
- Plans adjusted payment rate: $800 pmpm ($9600 per year)
- Darlene: Congestive Heart Failure, Diabetes with complications, Diabetic Proliferative Retinopathy, Hip Fracture
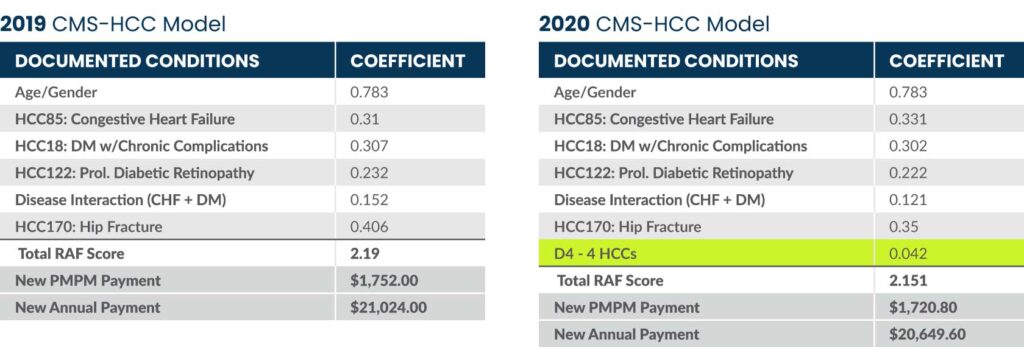
The chart above shows the difference in payment between the 2019 and 2020 models. For CY21 the rate will be blended 25/75 between the two models with the new risk adjustment being fully phased-in by CY22. While the announcement January 6th is a draft and will be finalized in April, this Notice continues CMS’ trend to be more conservative in the payment models.
What This Means for Health Plans
Plans need to continuously optimize their models for the most favorable risk adjustment revenue. It’s important for plans to get information, as quickly as possible, that may impact their risk adjustment scores. Health Risk Assessment (HRA) questionnaires continue to be an effective way to capture this information early so plans can influence adjustments in their CMS payment and effectively manage the member conditions.
Icario has helped clients administer HRAs to capture data relevant to an individual’s underlying health condition and status. This is especially critical early on so that the plan can proactively address a member’s health issue before the condition becomes larger impacting the member’s health and creating a costly claim.
HRAs can help a plan identify high risk individuals who may forego a doctor visit with such a tool enabling a more focused effort in driving care. This information can be accretive for risk adjustment purposes to continue to identify those at highest risk and being able to flag conditions for payment adjustments.

